From January 2001 to September 2004, preoperative cTnI was measured in 1,978 consecutive patients scheduled for isolated CABG. Preoperative cTnI values were available in 1,978 of 3,124 patients who fulfilled the inclusion criteria and in whom primary isolated CABG had been performed. Among these patients, negative preoperative cTnI levels ( 1.5 ng/mL) [Fig 1]. There were no significant differences between most perioperative patient characteristics of the remaining 1,146 CABG patients, who were initially not enrolled…
Tag: risk stratification
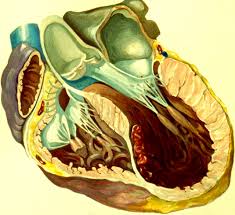
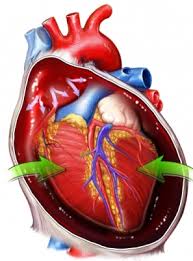
Cardiac Function
Clinical End Points The primary end point of the study was in-hospital mortality, defined as death from any cause within 30 days after surgery or during the same time period of hospitalization as well as postoperative MACE during the period of hospitalization including perioperative MI (PMI) and low cardiac output syndrome (LCOS). Secondary study end points were other postoperative complications such as stroke, new-onset ventricular arrhythmia , major bleeding, necessity for rethoracotomy, and postoperative renal failure requiring…